Where we’re Heading in Joint Care: Regeneration, AI Prediction and Evidence Translation
.png)
Joint care is on the verge of an evolutionary leap. Innovations in regenerative therapies, data-driven predictive tools and digital health technologies are changing how clinicians approach disease progression, intervention timing and long-term outcomes1. Healthcare providers working in primary care, Musculoskeletal (MSK) services and rehabilitation will need a clear understanding of these developments to support informed clinical decision-making.
Emerging Regenerative Approaches
A number of regenerative and biologically oriented therapies are being explored in joint care, aiming to modulate inflammation and promote tissue repair. The current landscape is summarised below.
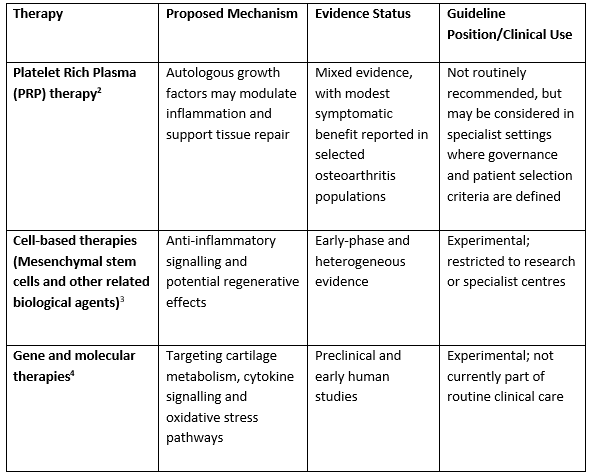
Across current clinical guidelines, regenerative therapies are positioned as adjuncts to established conservative management rather than replacements, with use generally confined to specialist or research settings.

![Artificial intelligence (AI) and machine learning models are increasingly being developed to help predict which patients are most likely to progress to severe disease or require joint replacement. These tools typically integrate demographic factors (i.e. age, sex), clinical data (i.e. pain severity, function scores), imaging features and metabolic and lifestyle risk factors.
Early studies suggest that AI models may outperform traditional risk stratification methods in predicting disease progression.[1] In the future, this could facilitate earlier referral of high-risk patients, more focussed use of imaging and interventions and more individualised follow-up intensity. However, clinical validation, transparency and integration into existing workflows remain major challenges that must be addressed before widespread implementation.](/images/pages/2258-1-3.webp)
